What is vitrectomy?
Vitrectomy is eye surgery to remove the vitreous (the gel that fills the eyeball). The procedure is also performed when it is necessary to remove the vitreous to work directly on the retina, even when the vitreous is in good condition. This surgery has enabled many patients, who a few years ago would have irretrievably lost their vision, to maintain or recover it to satisfactory levels.
When is it performed?
There are many ocular diseases that require vitrectomy, mainly retina related:
- Diabetic retinopaty
- Retinal Detachment
- Eye injury or trauma, diseases of the macula, macular holes or neovascular macular degeneration
- Secondary problems or eye inflammation
- Pathologies related to high myopia
- Occasionally, after cataract surgery when complications have arisen
What tests are necessary before surgery?
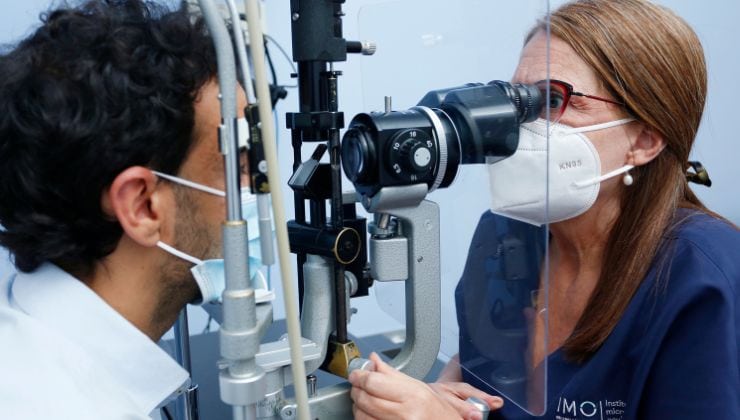
Before the procedure, a detailed eye examination, and often an ultrasound, is performed to determine the condition of the eye tissue. Other tests include:
- Retinal Optical Coherence Tomography (OCT): a scanner used to capture tomographic images of the eye in high definition
- Angiography: a contrast test to detect possible fluid loss or damage to blood vessels in the eye
- Electrophysiological test:a test that records electrical stimulation of the eye to detect problems in the retina and throughout the visual pathway to the cerebral cortex
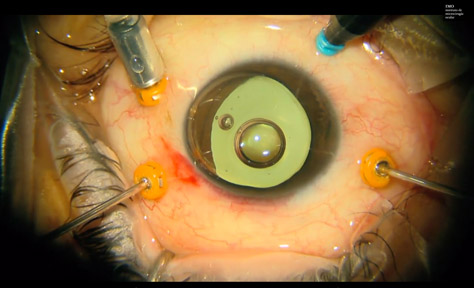
How is it performed?
Vitrectomy is the removal of the clear gel (vitreous) from the eye. The procedure is carried out with delicate instruments that are inserted into the eyeball through small incisions in its outer wall (sclera). Some of the instruments used include: a fibre optic light to illuminate the retina, an irrigation cannula to maintain intraocular pressure and an instrument that cuts and removes the vitreous. Also used are scissors, forceps and numerous other instruments selected for each operation. During surgery, the eye may receive an injection of gas or a gas and air mixture to repair a retinal detachment, close a macular hole or correct other defects. The procedure is performed under local anaesthesia and lasts one to two hours, depending on the condition of the eye. Occasionally, the ophthalmologist has to repair other tissue and perform other parallel procedures, such as removing a cataract or carrying out a corneal transplant.
After the surgery
Following surgery, the occlusion patch is usually removed after a few hours. The patient may have some pain in the eye, which should only be treated with eye drops and ointment to relieve the symptoms and intraocular inflammation. In general, postoperative patients can lead a normal life, except in cases where gas has been inserted into the eye during surgery. The gas is slowly absorbed by the eye over a period of time that may last several weeks depending on the type of gas used. When the eye is filled with gas, vision is very poor. As the gas is absorbed, various uncomfortable visual effects are produced, which eventually disappear completely. While the gas is dissolving, the patient should not fly or travel up to altitudes of 800-1000 metres rapidly. If this is unavoidable, it is advisable to consult with the ophthalmologist.
Risks
The risks of vitrectomy are by far outweighed by the benefits of improved vision after surgery. Some of the potential risks are postoperative bleeding, retinal detachment, increased ocular pressure after surgery, cataracts and infection.
Experts performing this treatment
FAQs
Yes, after any eye operation, although it is advisable to wait several days for the scars to heal. It normally takes ten to twelve days to return to a normal life. It is always best to consult the doctor to find out about the risk factors.
The symptoms of a detached retina are the presence of flashes of light (photopsia) or objects floating in the vitreous humour and, occasionally, a progressive shadow and loss of vision. It is important to contact your ophthalmologist as quickly as possible. It is not an emergency, but it needs to be operated on as soon as possible by a surgeon.
If a patient who has been operated on for cataracts or other intraocular processes suffers a severe loss of vision with noticeable eye redness and pain, he or she must go and see an ophthalmologist urgently and without delay, as the emergency could threaten the vision of the eye.
In general, the patient can lead a normal life, unless there is gas inside the eye, in which case the patient should heed the advice of his doctor. Flying above 600–800 m and travelling over high mountain passes, either by train or car, should be avoided. If such needs arise, the ophthalmologist should be consulted.
It is much more likely for haemorrhages to occur after surgery, especially if a vitrectomy has been performed, in the case of patients with diabetic retinopathy. This is due to the vessel walls being extremely fragile in these patients and more prone to bleeding.
The head should normally be tilted forward so that the gas does not contact the front of the eye, but the surface of the back of the eye. The length of time that the head should be kept in this position depends on the quantity of gas given.
If there is no gas or silicone oil, the patient can sleep in any position. If there is no covering element (gas or silicone oil), the patient’s position is unimportant.
Yes, it is an emergency, but relatively speaking, as it is possible to wait 3 or 4 days. It is necessary to examine the eye, because the symptom could indicate the onset of decompensation, which can cause severe loss of vision. This distortion is sometimes not due to decompensation, but it always needs to be confirmed.
When they have very little gas, i.e. one fifth or less in the eyeball, they can travel by air without a problem. If, however, they have a larger amount, they cannot fly, because the change in air pressure makes the gas bubble expand, which can cause ocular hypertension and damage the optic nerve.
IMO Institute of Ocular Microsurgery
Josep María Lladó, 3
08035 Barcelona
Phone: (+34) 934 000 700
E-mail: international@imo.es
See map on Google Maps
By car
GPS navigator coordinates:
41º 24’ 38” N – 02º 07’ 29” E
Exit 7 of the Ronda de Dalt (mountain side). The clinic has a car park with more than 200 parking spaces.
By bus
Autobus H2: Rotonda de Bellesguard, parada 1540
Autobus 196: Josep Maria Lladó-Bellesguard, parada 3191
Autobuses H2, 123, 196: Ronda de Dalt – Bellesguard, parada 0071
How to arrive at IMO from:
IMO Madrid
C/ Valle de Pinares Llanos, 3
28035 Madrid
Phone: (+34) 910 783 783
E-mail: administracion.madrid@imo.es
Public transport
Metro Lacoma (líne 7)
Autobuses:
- Lines 49 & 64, stop “Senda del Infante”
- Line N21, stop “Metro Lacoma”
Timetables
Patient care:
Monday to Friday, 8 a.m. to 9 p.m.
IMO Andorra
Av. de les Nacions Unides, 17
AD700 Escaldes-Engordany, Andorra
Phone: (+376) 688 55 44
See map in Google Maps