What is retinitis pigmentosa?
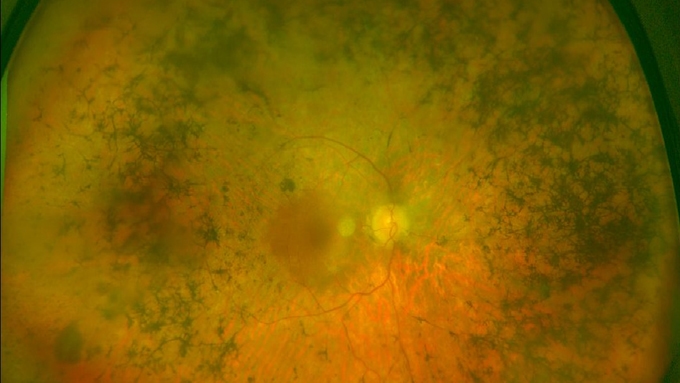
Retinitis pigmentosa is the most common hereditary disease of the retina that affects about 1 in every 4,000 people and is characterised by the gradual degeneration of the retinal photoreceptor cells: the cone and rod cells.
What causes this?
Due to the degeneration of the retinal photoreceptor cells, there is a gradual decrease in sight.
How can it be prevented?

There is no treatment at present and its seriousness makes it one of the ocular pathologies of genetic origin on which the most research is being conducted.
Symptoms
The first symptoms are night blindness or being unable to adapt to darkness and loss of peripheral vision, resulting in tunnel vision. In more advanced stages, glares and cataracts are also commonplace, which can appear as a consequence of the process.
Associated treatments
The degree of severity and progression that the pathology can reach is variable and depends on the mutated gene in each person and his/her family, because retinitis pigmentosa is a hereditary disease and it is therefore essential to know the patient’s family background. Finding the mutated gene in each case, from among more than 50 that can cause this pathology, requires a correct prior clinical diagnosis so that, in this way, customised and a precise genetic diagnosis can be made to determine the kind of heredity and transmission of the disease and identify the pre-symptomatic and carrier relatives.
The genetic diagnosis is also the first step required to apply gene therapies, based on replacing the defective gene with another functional one. Generally, these therapies are conducted by means of a modified virus that contains the functional gene and acts as a vector to be inserted in the patient’s retinal cells. Although still in an experimental stage, gene therapies are showing very encouraging results and are opening a new possibility for patients suffering from retinitis pigmentosa, a disease that has no cure at the moment.
Another of the research lines in process is cell therapy, one of the main novelties presented at the II Trends in Surgical & Medical Retina. As explained by the North American doctor, Marco Zarbin, at the international congress held at IMO last June, recent phase I studies on humans have proven that the use of stem cells to replace damaged cells of the retina leads to improvement of patients’ visual acuity. Therefore, what is being achieved with this therapy is the replacement of the patient’s atrophic photoreceptor cells, which will not be regenerated, for embryonic or pluripotent stem cells extracted from the skin or other parts of the eye. The latter, after being modified, can perform the same function as the retinal cells before they were damaged.
Specialists who treat this pathology
FAQs
Angiography is a technique used to delineate retinal or choroidal cases. Different contrasts are used, usually sodium fluorescein or indocyanine green. The scan is also useful for the diagnosis of other retinal diseases, such as pigment epithelium. In general, angiography is used to study many retinal diseases and their diagnosis.
It is a diagnostic technique to determine pathological and abnormal structures in the blood vessels and the different layers of the retina. It can be used in cases of macular degeneration, diabetic retinopathy, vasculopathy and many other macular disorders.
Age-related macular degeneration is one of the greatest challenges in ophthalmology today. We know that there are two types: the dry form and the wet form. The dry form is experienced by patients who are slowly losing their vision. It has been demonstrated that treatment with antioxidants and vitamins can reduce vision loss, although the slowing down of the process is not particularly spectacular. The wet form, which is so called because fluid is produced in the macula, is the most destructive, and current treatment involves the combining of photodynamic therapy, which started to be used some years ago, with other treatments, which has produced more positive results. Each year, new possibilities appear, which help in the fight against this disease.
IMO Institute of Ocular Microsurgery
Josep María Lladó, 3
08035 Barcelona
Phone: (+34) 934 000 700
E-mail: international@imo.es
See map on Google Maps
By car
GPS navigator coordinates:
41º 24’ 38” N – 02º 07’ 29” E
Exit 7 of the Ronda de Dalt (mountain side). The clinic has a car park with more than 200 parking spaces.
By bus
Autobus H2: Rotonda de Bellesguard, parada 1540
Autobus 196: Josep Maria Lladó-Bellesguard, parada 3191
Autobuses H2, 123, 196: Ronda de Dalt – Bellesguard, parada 0071
How to arrive at IMO from:
IMO Madrid
C/ Valle de Pinares Llanos, 3
28035 Madrid
Phone: (+34) 910 783 783
E-mail: administracion.madrid@imo.es
Public transport
Metro Lacoma (líne 7)
Autobuses:
- Lines 49 & 64, stop “Senda del Infante”
- Line N21, stop “Metro Lacoma”
Timetables
Patient care:
Monday to Friday, 8 a.m. to 9 p.m.
IMO Andorra
Av. de les Nacions Unides, 17
AD700 Escaldes-Engordany, Andorra
Phone: (+376) 688 55 44
See map in Google Maps