Family history and eye health
12 de April de 2022
How can it affect your eye health?
A large number of eye diseases are genetic in origin. Finding out about the eyesight problems of your parents, grandparents and other direct relatives and acting accordingly, through regular eye check-ups, is a good way of preventing molecular eye disorders from ultimately hindering our everyday activity.
On what does the degree of damage depend?
Genetic diseases are transmitted within the family and are caused by the alteration/mutation of a several gene. Transmission of the disorder may follow different inheritance patterns: dominant, recessive or X-linked. In each case, the likelihood of transmitting the disease will be different.
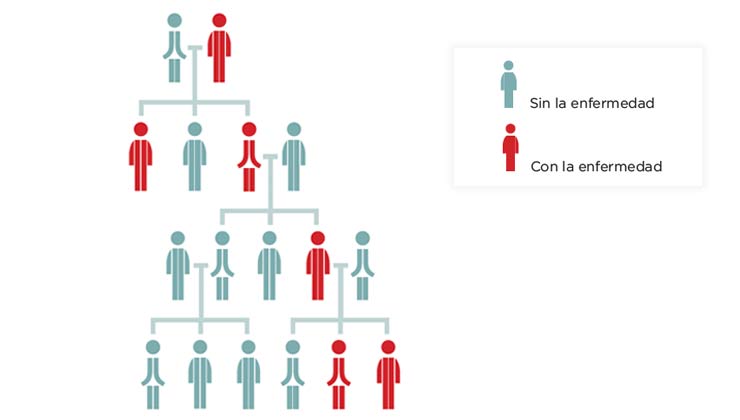
Dominant inheritance
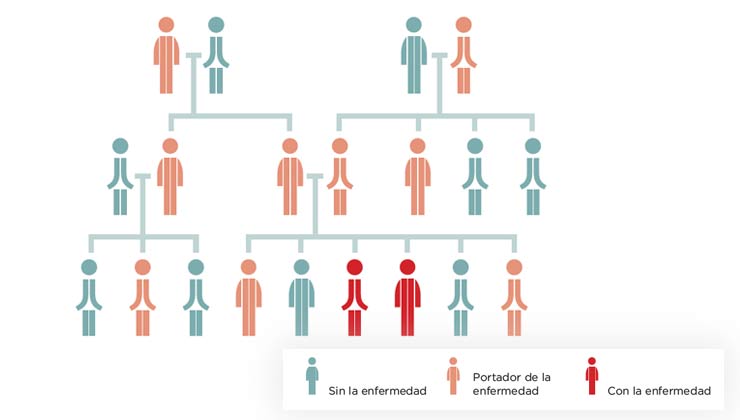
There are relatives from all generations in this inheritance pattern who suffer from the disorder, and these transmit the disease to 50% of their descendants. People with a dominant inheritance pattern and carriers of the gene mutation suffer from the disease.
Some examples of ophthalmological diseases with a dominant inheritance pattern are:
- Aniridia.
- Best disease.
- Blepharophimosis.
- Retinitis pigmentosa.
Recessive inheritance
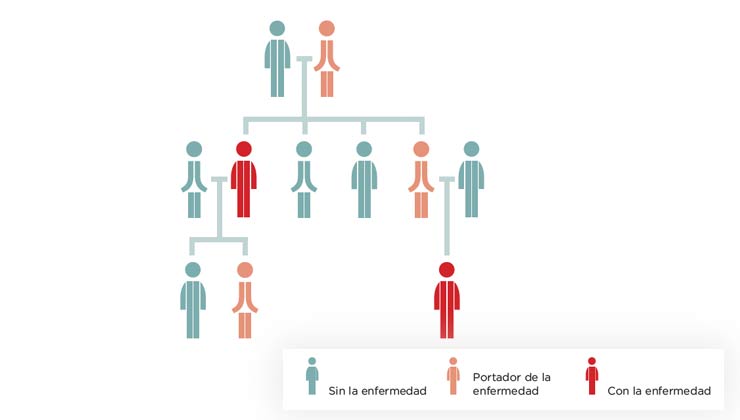
In this inheritance pattern, the relatives affected are in just one generation and the relatives who are carriers of the gene mutation do not suffer from the disease.
Some examples of ophthalmological diseases with a recessive inheritance pattern are:
- Stargardt disease
- Usher Syndrome.
- Retinitis pigmentosa.
X-linked inheritance
In this inheritance pattern, mothers are carriers of the gene mutation and transmit it to their sons.
Some examples of ophthalmological diseases with an X-linked inheritance pattern are:
- Choroideremia.
- Norrie Disease.
- Retinoschisis.
- Retinitis pigmentosa
Ophthalmic genetic diagnosis and counselling at IMO
IMO offers a genetic diagnosis service involving 30 hereditary eye disorders. Based on a blood sample from the patient and their relatives, the IMO molecular biology laboratory, coordinated by Dr Esther Pomares, identifies the molecular causes and supplements the clinical diagnosis.
The information collected means that genetic counselling can be offered to the family, identifying the inheritance pattern of the disorder and indicating the likelihood of its transmission, alerting asymptomatic patients and providing an estimated prognosis of the disease (how it will evolve). This lays the foundation for the early, effective application of future gene therapies that are currently at any advanced stage of study and that, over the coming decade, will allow for disorders to be treated for which there is currently no known cure.
How is it performed?
- Firstly, a clinical diagnosis is required from the ophthalmologist.
- Then, by appointment, a geneticist is seen to go over the family clinical history and draw up the family tree.
- All this information is used to identify the inheritance pattern of the disorder, which will determine the genes to be analysed.
- After this, genomic DNA is extracted from a blood sample provided by the patient and his or her relatives.
- In the laboratory, once the DNA is purified, the relevant genes are directly sequenced (those that are described as being responsible for certain familial disease) to identify the mutation or pathogenic abnormality. This process can take between 3 and 6 months.
- Finally, the patient is given the report and is offered genetic counselling for him/her and his/her relatives.
What is it for?
- To support and confirm the clinical diagnosis, as some visual alterations with overlapping symptoms are very difficult to diagnose.
- To determine the prognosis of the disease (know how it will evolve), which has a direct impact on patient expectations and treatment, while avoiding confusion and unsuitable therapies.
- To offer genetic counselling to families, identifying the disorder’s pattern of inheritance and revealing the likelihood of transmitting it.
- To alert family members who are carriers to the fact that they have not yet developed the disease but are very likely to suffer from it in the future.
- To prepare candidates for gene therapies, currently in an advanced study phase and that will allow these disorders with no current cure to be treated over the next decade.
- To obtain a greater and better understanding of the disease, identifying new genes responsible for different disorders and new risk factors not previous associated.
IMO Institute of Ocular Microsurgery
Josep María Lladó, 3
08035 Barcelona
Phone: (+34) 934 000 700
E-mail: international@imo.es
See map on Google Maps
By car
GPS navigator coordinates:
41º 24’ 38” N – 02º 07’ 29” E
Exit 7 of the Ronda de Dalt (mountain side). The clinic has a car park with more than 200 parking spaces.
By bus
Autobus H2: Rotonda de Bellesguard, parada 1540
Autobus 196: Josep Maria Lladó-Bellesguard, parada 3191
Autobuses H2, 123, 196: Ronda de Dalt – Bellesguard, parada 0071
How to arrive at IMO from:
IMO Madrid
C/ Valle de Pinares Llanos, 3
28035 Madrid
Phone: (+34) 910 783 783
E-mail: administracion.madrid@imo.es
Public transport
Metro Lacoma (líne 7)
Autobuses:
- Lines 49 & 64, stop “Senda del Infante”
- Line N21, stop “Metro Lacoma”
Timetables
Patient care:
Monday to Friday, 8 a.m. to 9 p.m.
IMO Andorra
Av. de les Nacions Unides, 17
AD700 Escaldes-Engordany, Andorra
Phone: (+376) 688 55 44
See map in Google Maps