Allow us to explain how diabetes affects your eyesight
29 de October de 2021
On the occasion of World Diabetes Day, our experts offer a warning regarding the sudden loss of vision that diabetes can cause in the absence of proper control by an ophthalmologist.
The most serious consequence of diabetes for the eyesight is diabetic retinopathy (DED), which currently affects 50% of diabetics between the ages of 40 and 59 and around 70% between the ages of 60 and 79.
How does poor diabetes control affect the eyesight?
One of the main problems is that, while it may already be at a very advanced stage, DED gives no warning:
- There is no pain.
- There is no obvious visual impairment.
The result being that the patient may lose their vision all of a sudden.

The key aspect of diabetes is that it causes damage to retinal blood vessels and, without proper monitoring by a specialist, will progress to its most severe type: Proliferative Diabetic Retinopathy
Dr. Carlos Mateo, surgeon with more than 35 years’ experience in retinal diseases
Proliferative Diabetic Retinopathy is characterised by abnormal growth in retinal blood vessels, which can lead to serious vision problems, such as:
- Haemorrhages inside the eye (these are not visible externally but cause vision loss, in many cases severe).
- Retinal detachment.
Fortunately, “nowadays, in countries such as ours, while patients with diabetes tend to have the disease well under control we still find cases in which the most severe types of DED develop as a result of patients not following the instructions of endocrinology specialists“, the ophthalmologist points out.
Objective: an early approach to DED
Ideally, when approaching a patient with DED, we should “not to let the disease progress to the proliferative stage, because, at that point, surgery is already a necessity, given the seriousness of the condition in which the patient arrives at the clinic, and total or partial recovery of vision is more difficult. This is why we always insist on the importance of prevention via check-ups and metabolic control of the disease,” explains Mateo.
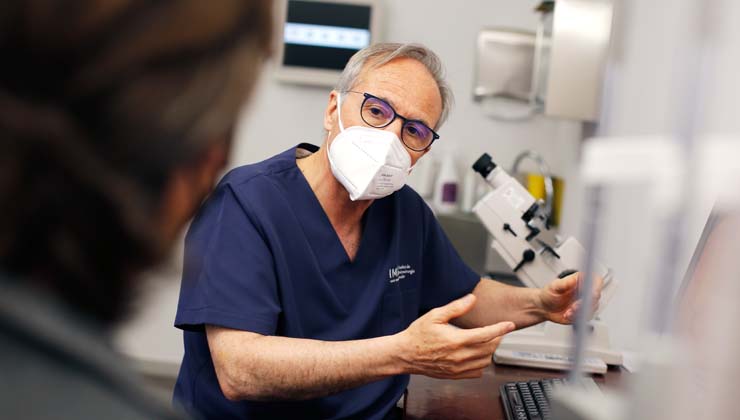
Follow-up ophthalmological visits are a key factor in early detection of diabetic retinopathy and its complications.
For less serious cases, other less invasive techniques are available, such as:
- Injections of drugs into the eye (intravitreal)
- Laser treatment
However, “each case must be assessed on an individual basis by an ophthalmologist with retinal expertise who can offer a personalised solution”, concludes Dr. Mateo.
3 key points for keeping diabetes under control

Check-ups with an endocrinologist and an ophthalmologist and correct adherence to specialist guidelines are crucial for good diabetes control.
According to Dr. Carlos Mateo, good diabetes control should be based on three points:
- Periodical check-ups with an endocrinologist.
- Visits to an ophthalmologist, depending on the degree of DED, at least once a year.
- A pro-active attitude on the part of the patient with regard to following the indications of their doctors.
Along the same lines, Type 1 diabetics (generally young people) should visit their ophthalmologist 8 years after diagnosis, and Type 2 diabetics (most of them adults) as soon as they are diagnosed.
IMO Institute of Ocular Microsurgery
Josep María Lladó, 3
08035 Barcelona
Phone: (+34) 934 000 700
E-mail: international@imo.es
See map on Google Maps
By car
GPS navigator coordinates:
41º 24’ 38” N – 02º 07’ 29” E
Exit 7 of the Ronda de Dalt (mountain side). The clinic has a car park with more than 200 parking spaces.
By bus
Autobus H2: Rotonda de Bellesguard, parada 1540
Autobus 196: Josep Maria Lladó-Bellesguard, parada 3191
Autobuses H2, 123, 196: Ronda de Dalt – Bellesguard, parada 0071
How to arrive at IMO from:
IMO Madrid
C/ Valle de Pinares Llanos, 3
28035 Madrid
Phone: (+34) 910 783 783
E-mail: administracion.madrid@imo.es
Public transport
Metro Lacoma (líne 7)
Autobuses:
- Lines 49 & 64, stop “Senda del Infante”
- Line N21, stop “Metro Lacoma”
Timetables
Patient care:
Monday to Friday, 8 a.m. to 9 p.m.
IMO Andorra
Av. de les Nacions Unides, 17
AD700 Escaldes-Engordany, Andorra
Phone: (+376) 688 55 44
See map in Google Maps