Noticias
No te pierdas todas nuestras novedades y los mejores contenidos para cuidar tu bienestar ocular.
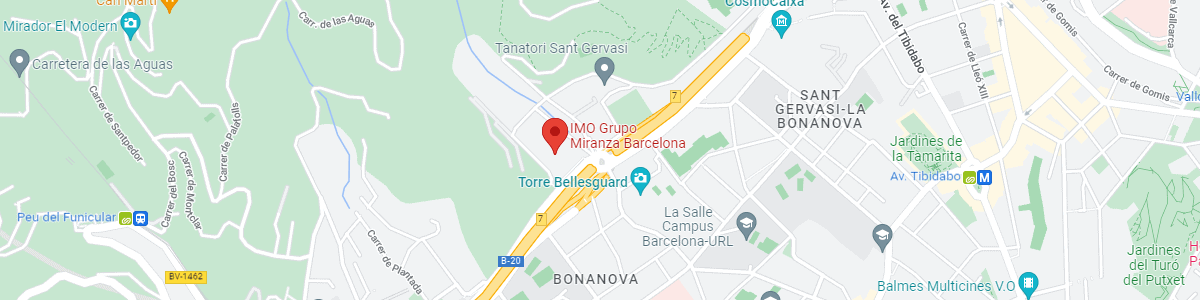
IMO Grupo Miranza Barcelona
Josep María Lladó, 3
08035 Barcelona
Tel: 934 000 700
E-mail: informacion@imo.es
Ver mapa en Google Maps
En coche
Coordenadas navegador GPS:
41º 24’ 38” N – 02º 07’ 29” E
Salida 7 de la Ronda de Dalt (lado montaña). La clínica cuenta con un aparcamiento de más de 200 plazas.
En bus
Autobús H2: Rotonda de Bellesguard, parada 1540
Autobús 196: Josep Maria Lladó-Bellesguard, parada 3191
Autobuses H2, 123, 196: Ronda de Dalt – Bellesguard, parada 0071
Cómo llegar a IMO desde:
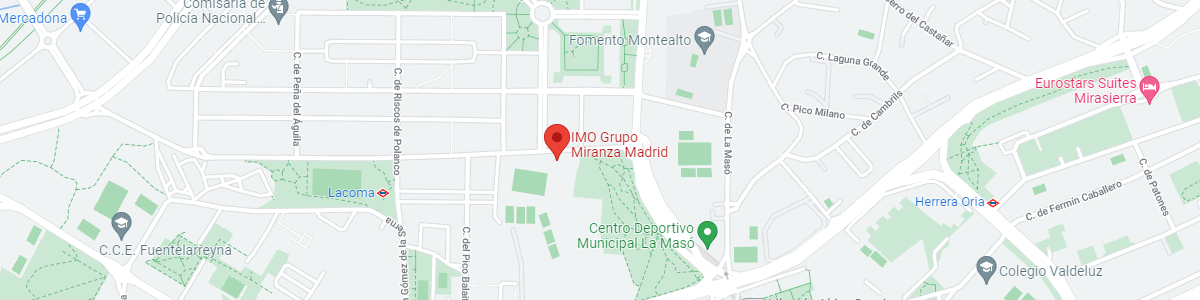
IMO Grupo Miranza Madrid
C/ Valle de Pinares Llanos, 3
28035 Madrid
Tel: 910 783 783
Ver mapa en Google Maps
Transporte público
Metro Lacoma (línea 7)
Autobuses:
- Líneas 49 y 64, parada “Senda del Infante”
- Línea N21, parada “Metro Lacoma”
Horarios
Atención al paciente: de lunes a viernes, de 8 h a 20 h
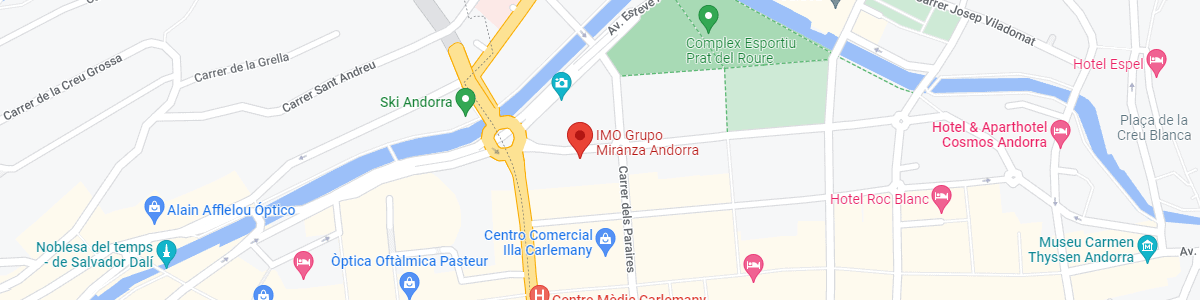
IMO Grupo Miranza Andorra
Av. de les Nacions Unides, 17
AD700 Escaldes-Engordany, Andorra
Tel: (+376) 88 55 44
Ver mapa en Google Maps
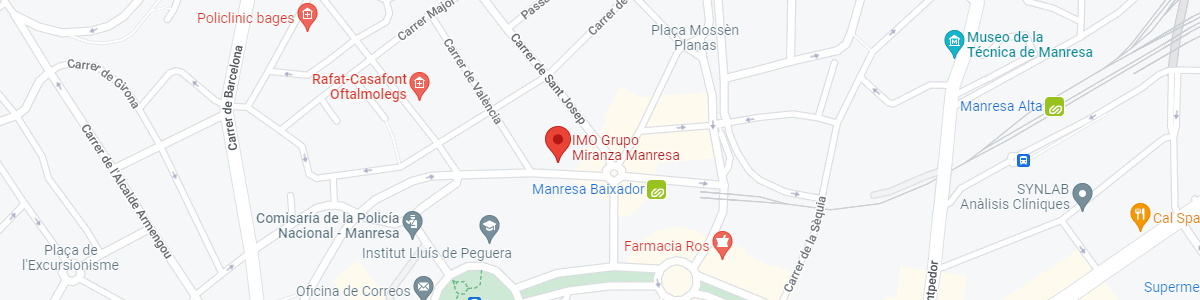
IMO Grupo Miranza Manresa
C/ Carrasco i Formiguera, 33 (Baixos)
08242 – Manresa
Tel: 938 749 160
Ver mapa en Google Maps
Transporte público
FGC. Línea R5 y R50 dirección Manresa. Estación: Baixador de Manresa
Horarios
De Lunes a viernes de 9:00 a 13:00 i de 15:00 a 20:00 h